How to Access Covered Care
Choose your doctor or change your doctor. Anytime.
With the Kaiser Permanente Added Choice® plan, you have a broad selection of providers to choose from.
Added Choice® lets you choose to receive covered services from KP Select Providers, PPO Providers, or Non-Participating Providers. The services we cover, and what you pay, will differ depending on the provider you choose.
To know if your plan allows for cross-accumulation between these providers for your deductible and out-of-pocket-maximum, see your Evidence of Coverage. Get more information on managing your deductible plan.
KP Select Providers
Kaiser Permanente Providers
Many ways to access care with KP Select Providers.
- Your care with KP Select Providers starts with your primary care physician who will help coordinate your care. You choose your own doctor, and you can change your doctor at any time.
- Choose a provider from Kaiser Permanente or The Portland Clinic, conveniently located throughout our service area. These providers have the lowest out-of-pocket costs.*
- You can manage your care at kp.org. Log in anytime from anywhere to make routine appointments, refill most prescriptions, see most lab results, and much more.
- Video or telephone visits with a doctor are available at no extra cost to most Added Choice® members. Members with a health savings account (HSA)–qualified high-deductible health plan (HDHP) will pay a fee for scheduled phone and video visits subject to your plan’s deductible.
* A referral may be required for Select Providers.
PPO Providers
First Choice Health or First Health Network
We provide many ways to access care through Participating Providers.
You have access to First Choice Health or First Health Network nationwide.
To find a Participating PPO Provider or confirm if your select PPO Provider is part of the network, please visit our customized provider locators.
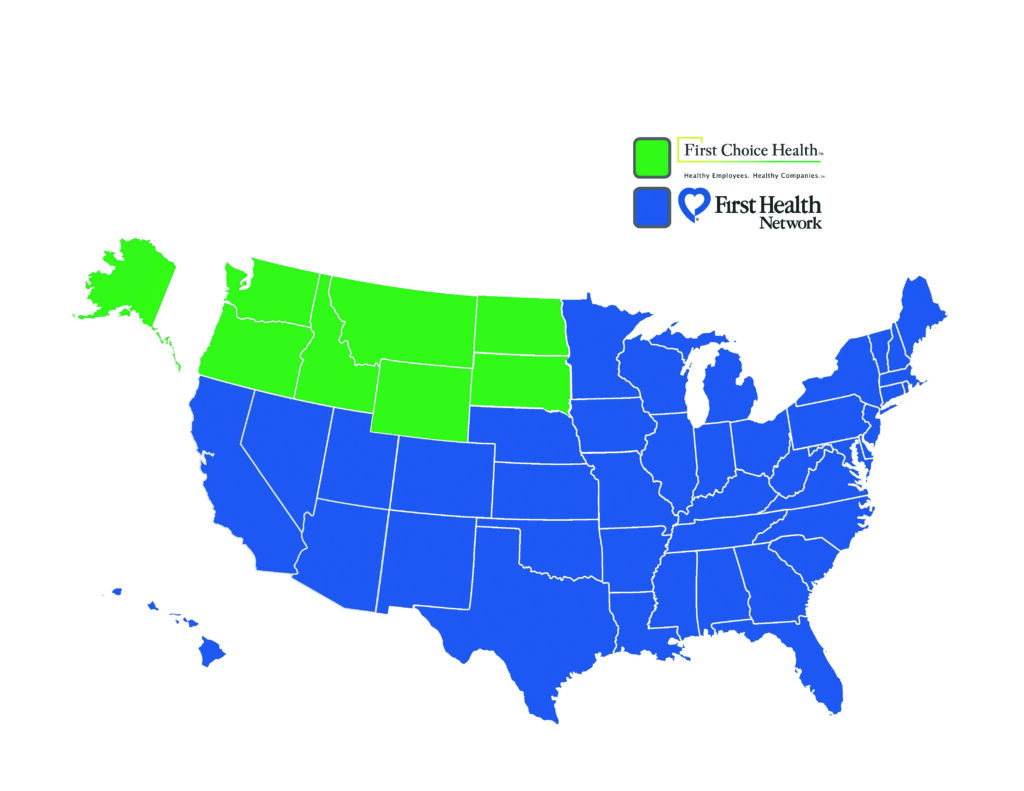
First Choice Health Network
(Members receiving care in OR, WA, ID, MT, WY, ND, SD, and AK.)
First Health Network
(Members receiving care in all states EXCEPT OR, WA, ID, MT, WY, ND, SD, and AK.)
- Most First Choice Health or First Health providers do not require a referral for specialty care. However, this is determined by the specialty provider so please inquire with them when scheduling your appointment. You will need prior authorization for some services and procedures. Your Participating Provider must call 1-855-281-1840 (TTY 711) for prior authorization. Failure to get prior authorization will result in greater cost to you.
- It is always a good idea to call the provider’s office to confirm they are a Participating Provider.
Can I nominate a physician to become a PPO provider?
- Yes. If you were seeing a doctor who is not a member of the First Choice Health or First Health Network before you became a member, you can nominate that doctor to become a participating PPO Provider. Please keep in mind your provider may choose not to participate.
- To nominate a provider, contact Customer Service at 1-866-616-0047 (TTY 711).
- Review can take up to 6 months. Whether a physician or practitioner is accepted depends on a number of considerations including the provider’s interest in joining, so a nomination doesn’t guarantee acceptance.
Helpful Tips
- When making an appointment. Make sure the PPO Provider is a Participating Provider (that is, part of First Choice Health or First Health Network) and is accepting new patients.
- When checking in for your visit. Bring your Added Choice® ID card with you. If your PPO Provider has any questions, have them call the Customer Service phone number on your ID card. All referrals should be to Participating Providers.
You can request your provider send lab, X-rays, and special procedure (MRIs, CT scans, PET scans, nuclear medicine) orders to a Kaiser Permanente facility. Once complete, Kaiser Permanente can send the results to your Participating Provider. Contact an Added Choice® Navigator at 503-813-3981 for assistance or to learn more.
Non-participating Providers
Any other licensed provider or physician
Call any licensed provider’s office directly.
- Your Non-Participating Provider benefits cover care you receive from any other licensed provider (who is not a KP Select Provider or PPO Provider).
- You can call the provider’s office directly to make an appointment.
- Most providers do not require a referral for specialty care. However, this is determined by the Specialty Provider so please inquire with them when scheduling your appointment. You will need prior authorization for some services and procedures. You must call 1-855-281-1840 (TTY 711) for prior authorization.
- Your doctor may require you to pay the full cost of the visit. And you will need to submit claim forms and itemized bills for reimbursement.
When using a Non-Participating Provider or facility, you will be responsible for the amount you are billed above the maximum allowable charge set out in your Evidence of Coverage (EOC) — this is referred to as balance billing. These charges billed directly by your provider do not apply to your deductible or out-of-pocket maximum.
Helpful Tips
- When making an appointment. Make sure the provider understands that your plan allows you to see any licensed provider.
- When checking in for your visit. Bring your Added Choice ID card with you. If your provider has any questions, have them call the Customer Service phone number on your ID card.
After your visit. Some Non-Participating Providers will require you to submit the claim. You will be responsible for paying the cost difference in addition to your copay and coinsurance.
You’ll pay the most out-of-pocket costs when you receive services from a Non-Participating Provider or facility.
It’s important to keep in mind:
- The services we cover, and what you pay, will differ depending on the provider you choose.
To find out more:
- Refer to your Evidence of Coverage (EOC).
- Contact the human resources/benefits representative where you work, if your employer provides your coverage.
- Call Customer Service at 1-866-616-0047 (TTY 711).
Some services require prior authorization. For more information, see your Evidence of Coverage (EOC).
