Understanding Your Plan and Benefits
Added Choice® empowers you to make the best health care choice for you — wherever you are, and whenever you need care.
Added Choice® lets you choose to receive covered services from KP Select Providers, PPO Providers, or Non-Participating Providers. The services we cover, and what you pay, will differ depending on the provider you choose.
To know if your plan allows for cross-accumulation between these providers for your deductible and out-of-pocket-maximum, see your Evidence of Coverage.
Get more information on managing your deductible plan.
KP Select Providers
Kaiser Permanente Providers
Choose a provider from Kaiser Permanente.
Features and benefits of our plan:
- Out-of-pocket costs. With these providers, you’ll pay the least out of pocket, with a lower or no deductible.
- Coordinated care. Your primary care physician works closely with specialists, pharmacists, lab technicians, therapists, and many other professionals. They are all connected through your electronic medical record for a coordinated care experience.
- NW medical offices. Kaiser Permanente’s medical offices are located throughout the Northwest region with doctors, specialists, imaging, and in most locations, pharmacy and lab, all in one place.
- Emergency care. You are covered for emergency care anywhere, worldwide.
- Urgent care. Urgent care is available at Kaiser Permanente medical offices. Call the number on the back of your ID card to confirm locations and hours of operations.
- Hospital care. Kaiser Permanente has 2 hospitals in the Portland area and carefully selects contracted hospitals to partner with us in taking care of you.1
- Medical advice. When you call for medical advice, you will be connected with a professional who can help advise you and make appointments with one of our providers. You can get advice by calling the number on the back of your ID card.
- Lab services. Your results from tests done in Kaiser Permanente medical offices can be read (for most results) online soon after the lab completes your tests, sometimes the same day.
- Preventive care. That includes routine physicals, well-child visits, and certain screenings and tests (such as mammograms).
- Telehealth options. Email or schedule a phone or video visit with your Kaiser Permanente doctor– all for a $0 copay for most members.2
- Manage your health online. Use the convenient features of kp.org to manage your health.
- Email your doctor’s office with routine, nonurgent questions
- View most test results
- Schedule or cancel routine appointments
- Refill most prescriptions
- View past visits
- Find care options and urgent care locations near you
- Register at kp.org/registernow (Make sure to select your region.)
Your username and password can also be used on our mobile app.
To find out more about what is covered with KP Select Providers, see your Evidence of Coverage (EOC) or call Customer Service at 1-866-616-0047 (TTY 711).
1. These contracted hospitals are independently owned and operated and are not affiliated entities of Kaiser Permanente.
2. These features apply to care you get at Kaiser Permanente facilities. When appropriate and available. If you have an HSA-qualified deductible plan, you will need to pay the full charges for scheduled phone and video visits until you reach your deductible. Once you reach your deductible, your copay is $0 for scheduled phone and video visits.
PPO Providers
First Choice Health, First Health Network, and Cigna HealthcareSM PPO Network1
Choose a PPO Provider from First Choice Health, First Health Network or Cigna Healthcare PPO Network. This provider option is for members that wish to keep their current PPO Provider or who live outside our service area.
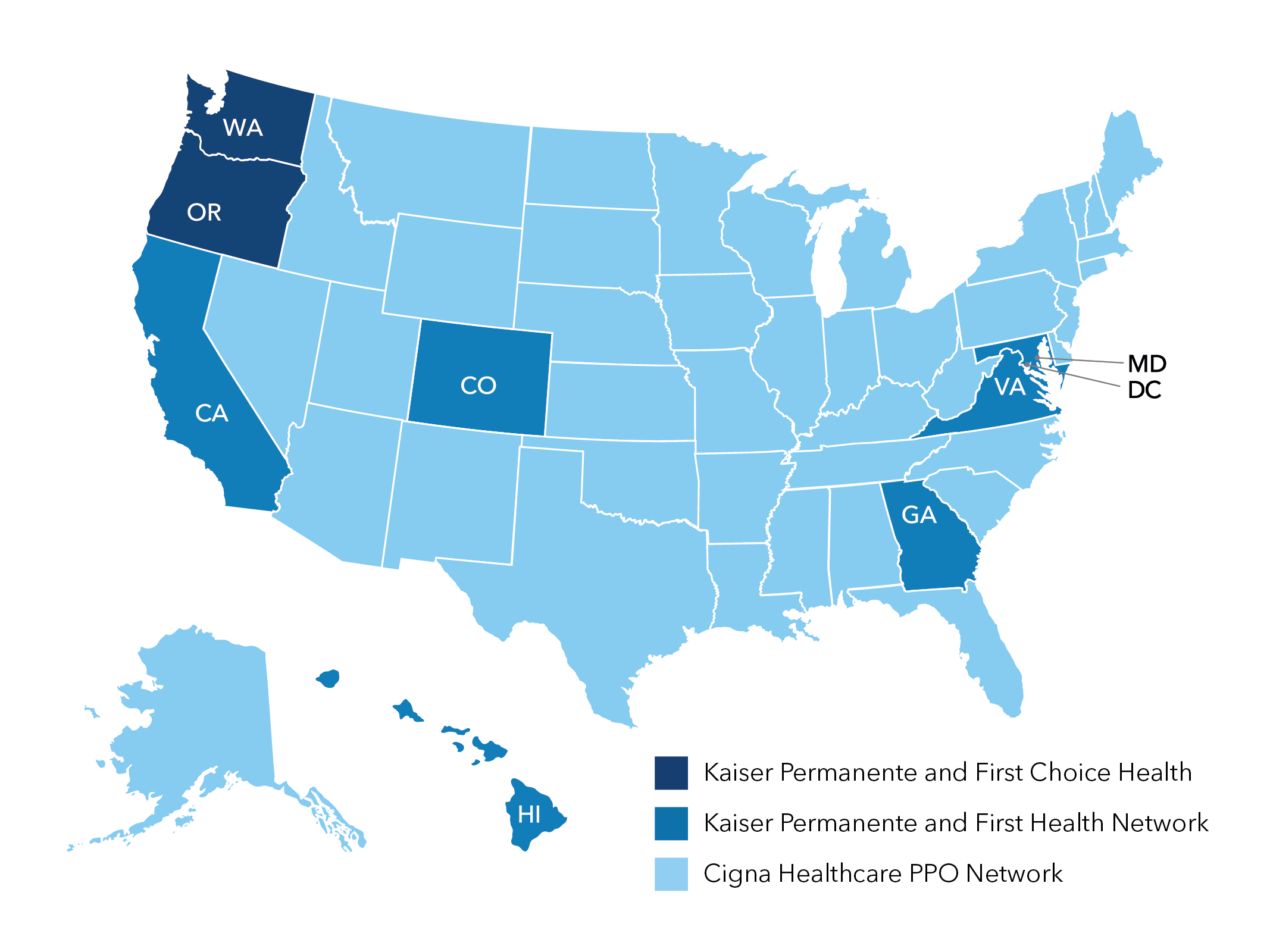
To find a PPO Provider or confirm if your current provider is part of the First Choice Health, First Health Network, or Cigna Healthcare PPO Network, please visit the link below or contact Customer Service at 1-866-616-0047.
First Choice Health
(Members receiving care in Oregon and Washington.)
First Health Network
(Members receiving care in California, Colorado, Georgia, Hawaii, Maryland, Virginia, and DC.)
Cigna HealthcareSM PPO Network
(Members receiving care in all other states.)
PPO Network Providers Nationwide. Depending on your service location, First Choice Health, First Health Network and Cigna Healthcare PPO Network is available to you. This nationwide network consists of doctors, hospitals, specialists and laboratories across the country.
- Out-of-pocket costs. You will have higher out-of-pocket costs with PPO Providers (such as a deductible, coinsurance, and a copayment) and in most cases you will not be responsible for the amount you are billed above the maximum allowable charge described in your Evidence of Coverage (EOC) — this is referred to as balance billing.
- Specialty care. Most PPO providers do not require a referral for specialty care. However, this is determined by the Specialty Provider so please inquire with them when scheduling your appointment. Your provider must obtain prior authorization for certain services and treatments2 such as:
- Inpatient hospital stay
- Outpatient surgery
- Home health, hospice, and skilled nursing facility services
- Imaging services
- Please review your Evidence of Coverage (EOC) for plan details
- Behavioral health. You can receive care for mental health and substance use concerns from a PPO Network provider.2
- Hospital care. You can receive inpatient hospitalization services from PPO Network hospitals and facilities. Your provider may make arrangements for your hospital admission.NOTE: Not all PPO Network Providers have admitting privileges with participating hospitals. Please confirm the facility and Provider is part of First Choice Health, First Health Network or Cigna Healthcare PPO Network.
- Maternity care. You can choose a PPO Network Provider for your obstetric care.
- Lab tests and imaging. You can choose a PPO Network Provider for lab tests and imaging.
- Pharmacy services. Learn about your pharmacy benefits on the Pharmacy page.
For additional information on what is covered with PPO Providers:
- Refer to your Evidence of Coverage (EOC).
- Contact the human resources/benefits representative where you work, if your employer provides your coverage.
- Call Customer Service at 1-866-616-0047 (TTY 711).
1. The Cigna Healthcare PPO Network refers to the health care providers (doctors, hospitals, specialists) contracted as part of the Cigna Healthcare PPO for Shared Administration.
Cigna HealthcareSM is an independent company and not affiliated with Kaiser Foundation Health Plan, Inc., and its subsidiary health plans. Access to the Cigna Healthcare PPO Network is available through Cigna Healthcare’s contractual relationship with the Kaiser Permanente health plans. The Cigna Healthcare PPO Network is provided exclusively by or through operating subsidiaries of The Cigna Group, including Cigna Health and Life Insurance Company. The Cigna Healthcare name, logo, and other marks are owned by Cigna Healthcare Intellectual Property, Inc.
2. Inpatient and certain outpatient services are subject to prior authorization. Your First Choice Health and First Health Network Providers must call 1-855-281-1840 (TTY 711) and Cigna Healthcare PPO Network providers must call 1-888-831-0761 for . Failure to get prior authorization may result in greater out-of-pocket cost to you.
This site provides an overview of your benefits and services. If there are any differences between this document and your Evidence of Coverage (EOC), your Evidence of Coverage (EOC) will prevail.
Kaiser Permanente has contracted with First Choice Health, First Health Network and Cigna Healthcare PPO Network. PPO Network providers are subject to change without notice.
Non-Participating Providers
Any other licensed provider or physician
Choose a Non-Participating Provider nationwide. Non-participating Providers include any licensed providers who are not KP Select or PPO Network providers. This provider option has the highest out-of-pocket costs.
Features and benefits of receiving covered care from any licensed provider:
- Provider choice, care anywhere. Your Non-Participating Provider benefits cover care you receive from any licensed provider (who’s not a KP Select or a PPO Network Provider).
- Using Non-Participating Providers means higher out-of-pocket costs. When using a Non-Participating Provider or facility, you may be responsible for the amount billed above the maximum allowable charge described in your Evidence of Coverage (EOC) — this is referred to as balance billing. These charges billed directly by your provider do not apply to your deductible or out-of-pocket maximum.
- Behavioral health. You can receive care from any licensed behavioral health or chemical dependency professional for mental health and substance use concerns.*
- Hospital care. You can receive inpatient hospitalization services from licensed or accredited hospitals and facilities that are not a KP Select or a PPO Network Provider.
- Emergency care. You can visit any licensed Non-Participating emergency care facility. Emergency care is covered at the same cost share as KP Select Providers.
- Urgent care. You can visit any licensed Non-Participating urgent care facility.
- Maternity care. You can choose any licensed provider for obstetric care.
- Lab tests and imaging. You can choose any licensed provider for lab tests and imaging.
- Pharmacy services. Learn about your pharmacy benefits on the pharmacy page.
For additional information on what is covered with Non-Participating Providers:
- Refer to your Evidence of Coverage (EOC).
- Contact the human resources/benefits representative where you work, if your employer provides your coverage.
- Call Customer Service at 1-866-616-0047 (TTY 711).
*Inpatient and certain outpatient services are subject to prior authorization. You or your provider must call 1-855-281-1840 (TTY 711) for prior authorization. Failure to get prior authorization may result in greater cost share to you.
This site provides an overview of your benefits and services. If there are any differences between this document and your Evidence of Coverage (EOC), your Evidence of Coverage (EOC) will prevail.
Balance Billing
If you use a Non-Participating Provider, or have services at an out of network facility, it is important that you understand balance billing. Balance billing can mean significant out-of-pocket costs for you.
Balance billing is the difference between what a Non-Participating Provider charges for a service and what Medicare will reimburse for that service. What Medicare will reimburse for the service is called an “allowed amount.”
For example, if a Non-Participating Provider charges $100 and the allowed amount is $70, the Provider may be able to balance-bill you directly for the difference — in this case, $30. You may be responsible for paying all amounts above the allowed amount in addition to your copay and coinsurance.
This is one reason why it’s generally less expensive to use KP Select and PPO Network providers. KP Select and PPO Network providers cannot bill you above the allowed amount.
Other things to know about balance billing:
- You can not be balanced billed for emergency services.
- You can not be balanced billed by an Out of Network Provider at certain In Network Facilities.
- Balance-billed amounts do not accumulate toward your deductible.
- Although your plan has an out-of-pocket maximum, it does not apply to balance-billed charges from a Non-Participating Provider. This means you could end up paying above your annual out-of-pocket maximum to cover the cost of a service.
- You could receive a bill in the mail at any time after your service.
Please contact Customer Service at 1-866-616-0047 (TTY 711) for more information.
